The Intelligent Operating System for Medical Benefit Prior Authorization
Unify, automate, and manage every medical benefit prior authorization in one system. SamaCare puts AI at your command, bringing intelligence from millions of real-world cases into your workflow to reduce delays and help patients start therapy faster.
Trusted by Practices Nationwide
Thousands of specialty practices across retina, oncology, neurology, rheumatology and infusion centers use SamaCare to manage medical benefit prior authorization.




One Intelligent System for Medical Benefit Prior Authorization
SamaCare brings every part of the medical benefit prior authorization process into a single system designed specifically for specialty practices.
Automate the Entire Prior Authorization Workflow
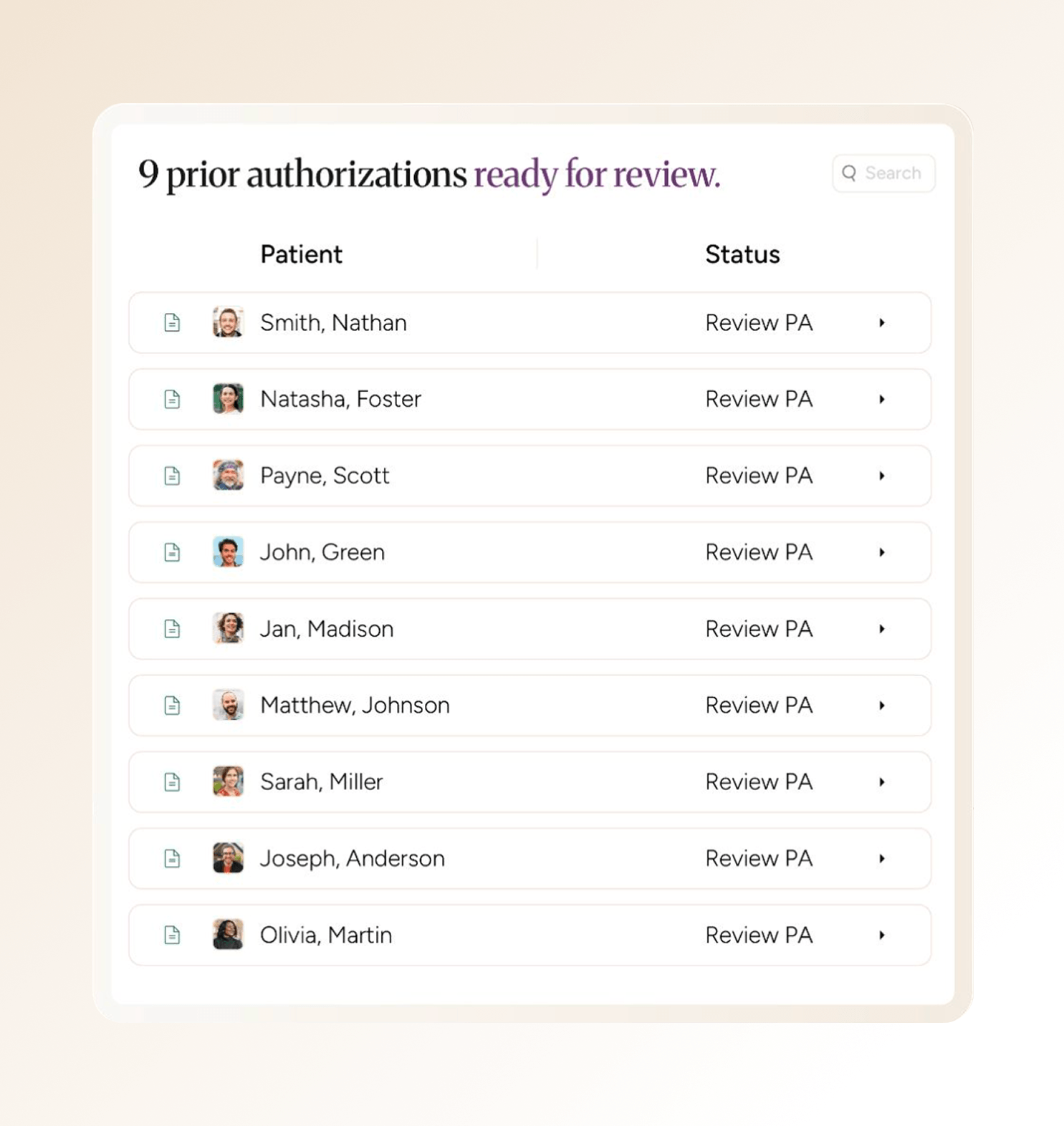
You shouldn’t have to spend your day clicking through forms and chasing payer portals. SamaCare automates prior authorization creation, submission, and follow-up so practices can handle more prior authorizations with the same team — and help patients start treatment sooner.
- Automatically create and submit prior authorizations individually or in bulk.
- Mitigate delays early with intelligent alerts and AI-to-human escalation.
- Stay in control with built-in checkpoints to make sure nothing goes out without your approval.

Get Approvals the First Time with Intelligent Workflows
Every prior authorization processed through SamaCare contributes to a growing network of real-world intelligence. By analyzing payer responses, submission outcomes, and workflow patterns across thousands of practices, SamaCare surfaces guidance to help staff navigate payer requirements effectively. Instead of guessing what documentation or steps may be required, practices receive recommendations informed by what really works across the network.
- Guided workflows optimized for approval.
- Pre-submission policy intelligence that surfaces the right forms, documentation, and requirements.
- AI recommendations in-workflow to help increase approval rates, reduce time to approval, and save staff time on PAs.

Gain Insights to Provide Better Care
When you’re not buried in busywork, it’s easier to see the big picture. SamaCare gives your practice a clear view of prior authorization performance across payers, therapies, and workflows — and how your results compare to peers across SamaCare’s network.
- Practice-level PA performance insights across payers, therapies, and submission pathways.
- Benchmarks to compare your approval rates and timelines to industry standards.
- Operational insights that help improve payer relations, allocate staff resources, and strengthen submission outcomes.
%20(1).png)
Built to Fit the Systems Practices Already Use
SamaCare integrates with the tools practices rely on every day, from EMRs to revenue cycle management systems. SamaCare also participates in industry standards initiatives, ensuring practices stay aligned with evolving payer and interoperability requirements.

.png)
.png)

Lessons From the SamaCare Network
What thousands of practices have learned about getting prior authorizations approved — shared in their own words, and built into the SamaCare platform.
"I would say the most complex part about the prior authorization process is probably finding out where to submit the authorization to."
"The number one reason I see for medical drug authorization denials is proof of medical necessity charting issues."
"My suggestion is to give them a call to find out if the patient has been approved or denied...instead of waiting for the decision to come in the mail."
Prior Authorization Resources for Specialty Practices
.svg)

.svg)
Automate Your Prior Authorization Workflow — with You in the Driver’s Seat
SamaCare combines intelligence from millions of prior authorizations with automation designed to support, not replace, human expertise. Practices gain the tools and insights needed to manage prior authorization more efficiently, improve approval outcomes, and help patients start therapy sooner.

.svg)